By M. Marin
NASDAQ:HIT
READ THE FULL HIT RESEARCH REPORT
Growing traction and adoption…
Health in Tech (NASDAQ:HIT), an insurance marketplace leveraging AI technology to introduce innovations within the self-funded healthcare insurance market and facilitate employers’ ability to obtain affordable health insurance, reported strong 3Q25 results this week.
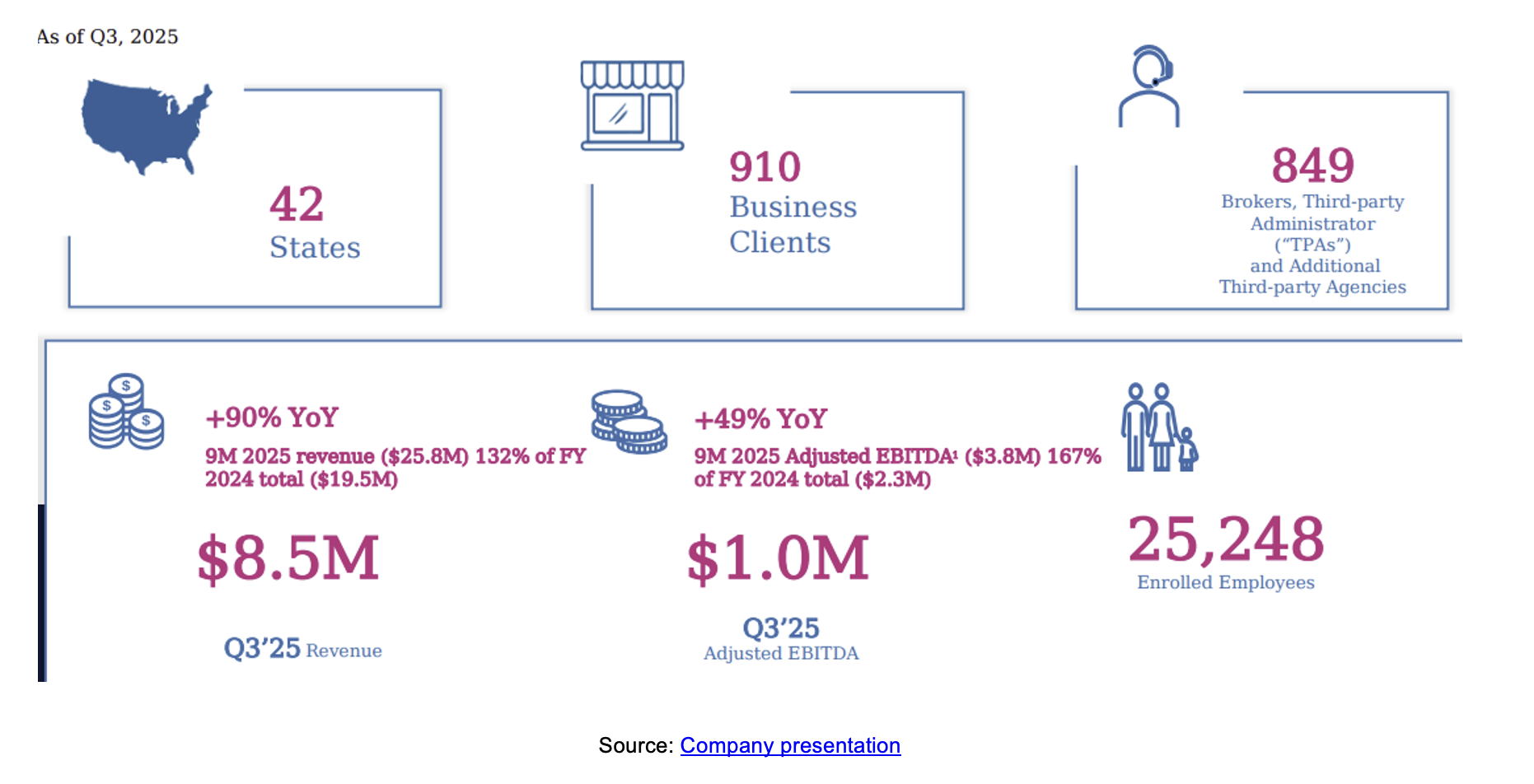
Revenue grew an impressive 90% year-over-year to $8.5 million, compared to $4.5 million in 3Q24. Cumulative revenue of $25.8 million in the first nine months of 2025 exceeds total full-year 2024 revenue of $19.5 million. Revenue growth is highly correlated with the number of enrolled employees (EEs) insured via its platform.
The number of EEs insured via its platform, therefore, is considered a critical indicator of growth and market penetration. The company bills service fees per EE on a monthly basis. In 3Q25, the company’s platform had 25,248 EEs billed for various services, up from 24,839 at the end of the prior quarter and up more than 40% compared to 3Q24. The company believes the increase in billed EEs reflects that HIT is expanding its market reach and seeing strong adoption across its growing network.
The company is benefiting from its strategy to expand its network and reach. For example, HIT’s distribution network expanded to 849 partners, up 57% year-over-year, reflecting the company’s strategy to extend the network beyond traditional broker channels, according to management, including partnerships with Third-party Administrators (TPAs), regional healthcare benefit providers and service platforms supporting small businesses.
New solutions & tools recently introduced and others under development, including solutions for larger employers, expand HIT’s target addressable market
HIT is leveraging its technology platform to introduce innovations and has recently introduced a key expansion of its Do-It-Yourself Benefit System (eDIYBS) to extend eDIYBS capabilities to the mid- and large-employer market and reduce quoting timelines significantly. With this upgrade, brokers who work with employers with 150 or more employees can upload claims files easily, and HIT's AI technology capabilities process the data quickly to generate bindable quotes for large employers in as short a time as two weeks, compared to what the company cites as the industry standard timeline that can frequently take up to three months. The company is extremely encouraged by the prospect of the large-employer underwriting within eDIYBS.
Concurrently, HIT continues to expand its offerings and reach for SMEs (the small and medium-sized enterprises), its legacy target addressable market (TAM). The majority of U.S. firms fall into this category, according to the U.S. Small Business Administration (SBA). The company believes the HIT platform can also make it easier for larger organizations to obtain insurance plans that are appropriate for their organizations. Reflecting interest it has generated to date, HIT is optimistic about the prospects for its AI-powered solutions for businesses of all sizes.
Planned 3-year rate hold solution
HIT anticipates continuing to introduce new enhancements such as the above-noted large-employer underwriting within eDIYBS, a planned 3-year rate hold for large-employers, and, longer term, blockchain-secured claims capabilities. For example, HIT is testing a 3-year rate hold to offer employers with 150 employees or more the benefit of predictable costs over a 3-year period. HIT expects to offset the impact of holding rates flat over a 3-year period with the efficiency of its technology-enhanced administrative processes. The company expects this solution to boost customer retention and provide additional offerings for its TPAs and other distribution partners. HIT expects to launch the 3-year rate hold solution in 1Q26.
Blockchain secured claims processing capabilities
HIT recently signed a non-binding strategic Letter of Intent (LOI) with digital asset treasury and blockchain infrastructure company AlphaTON Capital Corp. to combine their respective insurance expertise and blockchain infrastructure and security protocols to jointly develop a blockchain-enabled healthcare insurance claims processing platform built on The Open Network, HITChain. The JV partners expect HITChain to address inefficiency and fraud in the domestic healthcare claims processing space, lower administrative costs, and improve transparency.
SUBSCRIBE TO ZACKS SMALL CAP RESEARCH to receive our articles and reports emailed directly to you each morning. Please visit our website for additional information on Zacks SCR.
DISCLOSURE: Zacks SCR has received compensation from the issuer directly, from an investment manager, or from an investor relations consulting firm, engaged by the issuer, for providing research coverage for a period of no less than one year. Research articles, as seen here, are part of the service Zacks SCR provides and Zacks SCR receives payments totaling a maximum fee of up to $50,000 annually for these services provided to or regarding the issuer. Full Disclaimer HERE.